Blepharitis
Introduction
Blepharitis is an inflammatory condition that affects the eye lid margins. The edges of the eyelids become red and swollen1. It is a chronic condition which means that symptoms will reoccur if they are not managed. It may occur intermittently, and it is usually bilateral (meaning it affects both eyes).
Blepharitis is often used to refer specifically to ‘anterior blepharitis’, affecting the portion of the eyelid in front of the mucocutaneous junction. Posterior forms (affecting the portion behind the mucocutaneous junction), are typically identified according to their underlying cause, such as meibomian gland dysfunction (MGD)2. TFOS DEWS III classifies anterior blepharitis as “inflammation of the lid margin anterior to the grey line and concentrated around the eyelashes”3.
Both anterior and posterior blepharitis can coexist and have links to dry eye disease sharing similar clinical features2. It is important to remember that there is considerable overlap between anterior and posterior blepharitis (MGD).
The focus of the rest of this article will be on anterior blepharitis.
Blepharitis is the most common reason for same day cancellation of elective cataract surgery4. In research it has been linked with post operative endophthalmitis in cataract surgery where it was reported that the genetic makeup of organisms from the vitreous matched those recovered from the patient’s eyelids5.
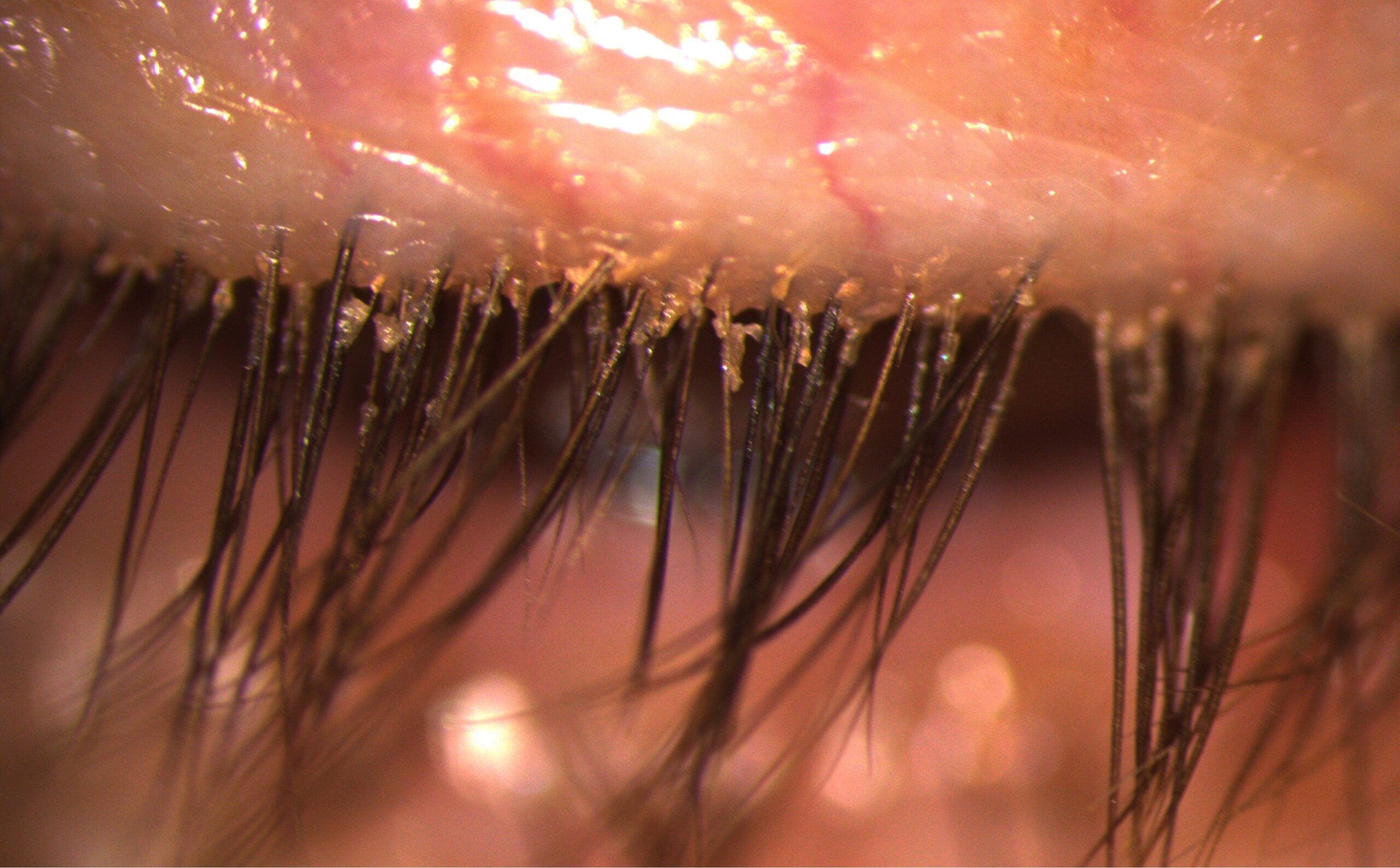
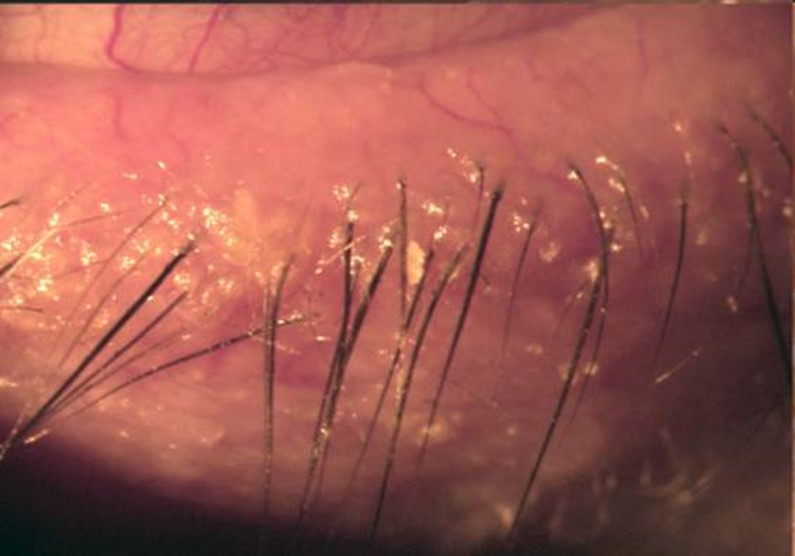
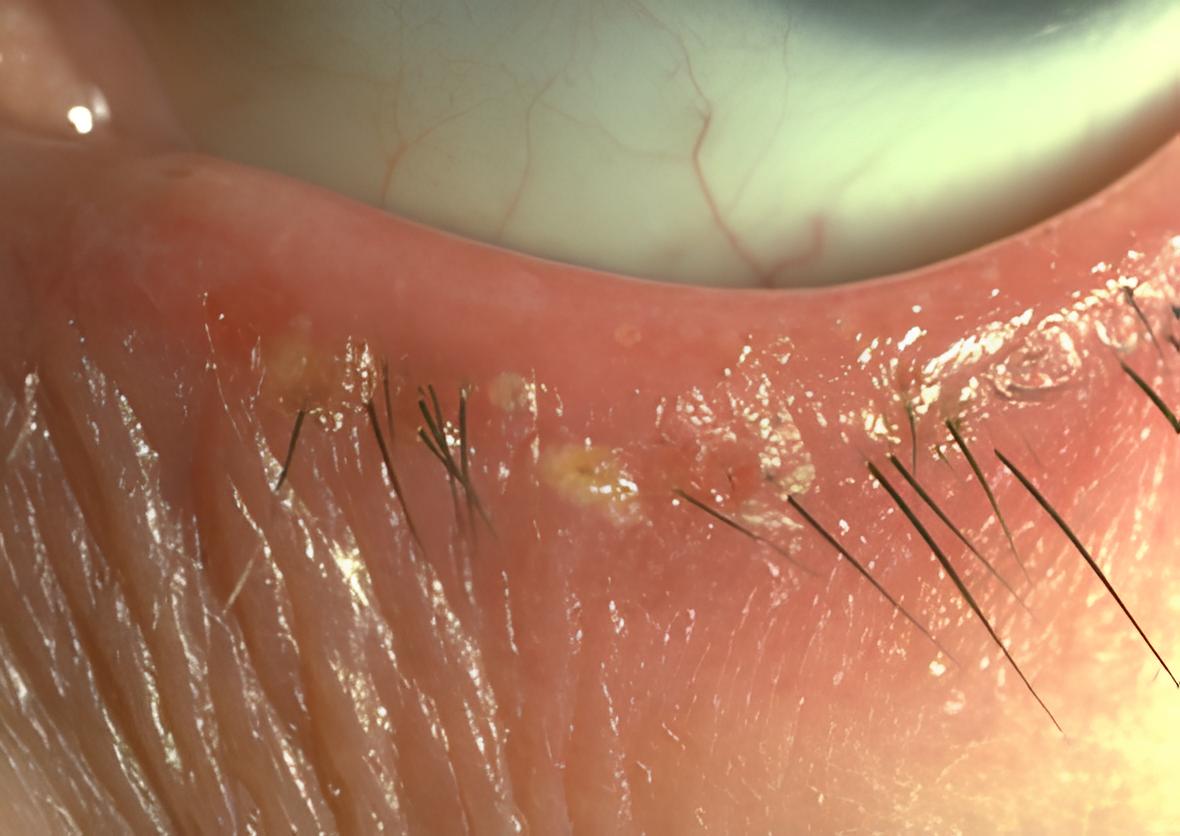
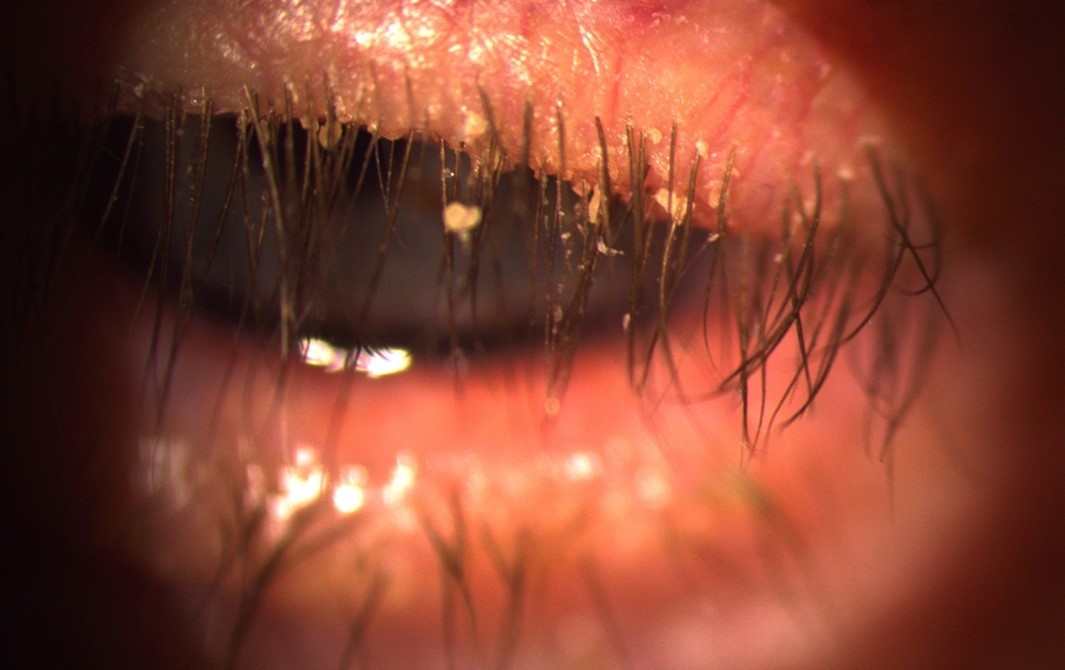
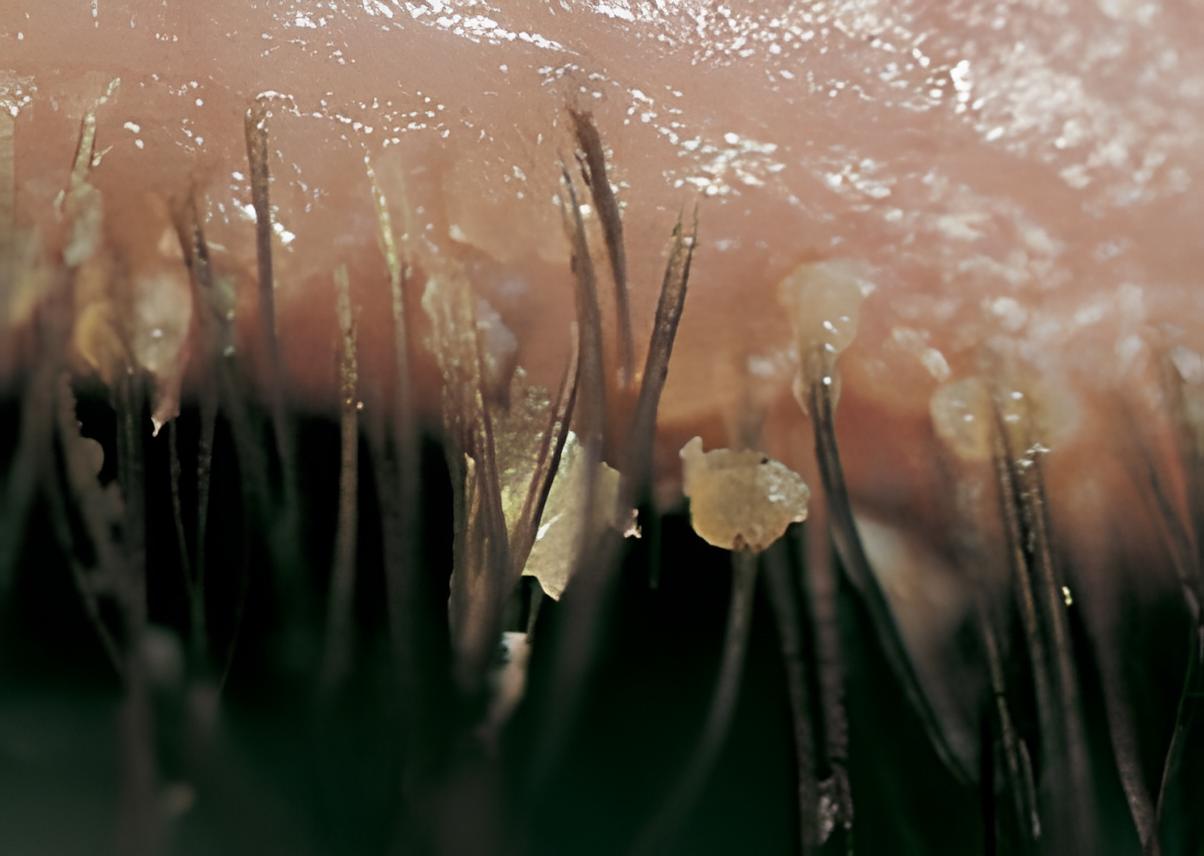
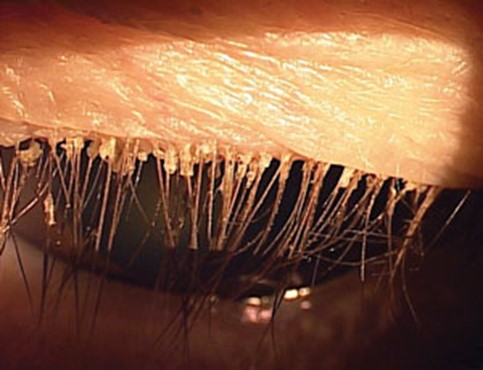
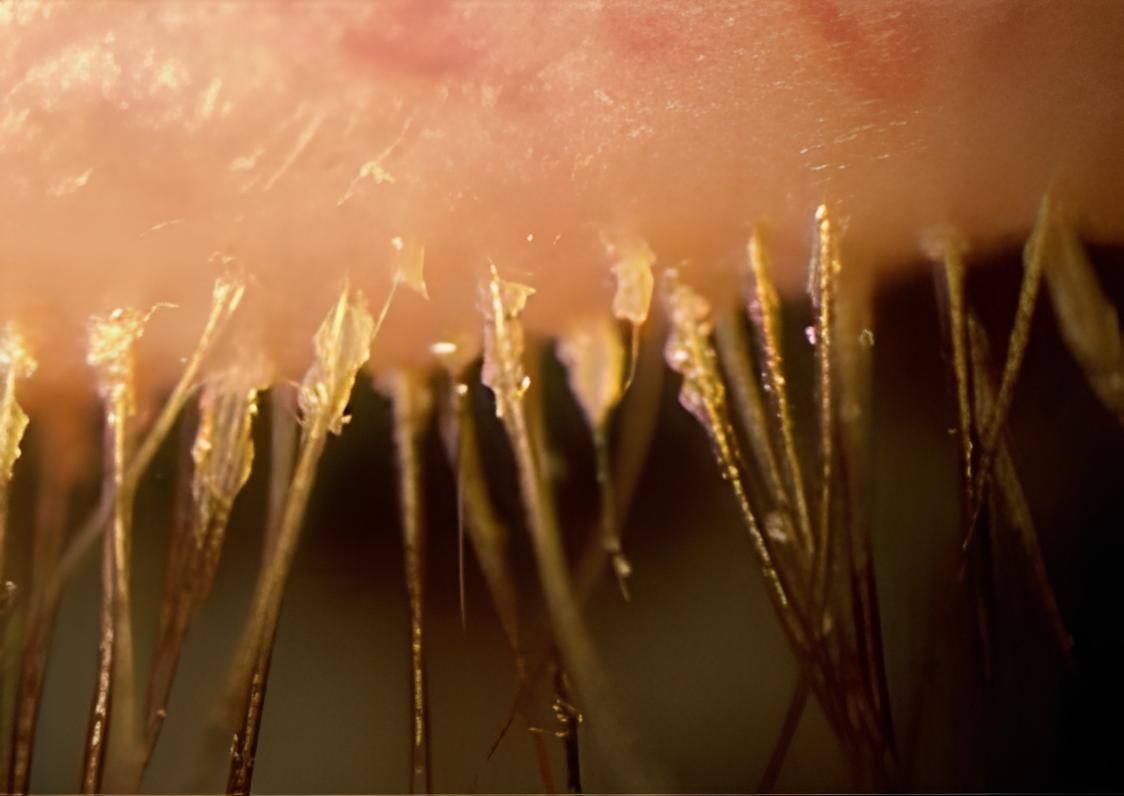
Anterior blepharitis primarily impacts the base of the eyelashes, targeting the eyelash follicles and the surrounding eyelid skin. In cases where the eyelid skin itself becomes inflamed, the term blepharo-dermatitis is used to describe this particular presentation.
The pathophysiology involves the accumulation of various substances, such as debris, bacteria, mites, or oils, along the eyelid margin. This build-up leads to irritation of the delicate skin of the eyelids and disrupts normal eyelid function, perpetuating the chronic nature of the condition.
It may present with:
- Crusting or flakes around lashes
- Red, irritated lid margins
- Itching, burning, or foreign‑body sensation
- Ocular surface discomfort and dry eye symptoms
Anterior blepharitis includes three key subtypes:
- Staphylococcal (bacterial)
- Seborrhoeic (oily imbalance – skin related)
- Demodex (mite‑related)
Each has different aetiological drivers (underlying causes), which is why identification matters.
Staphylococcal/Bacterial – this is caused by bacteria, normally staphylococcal by either
1) direct infection
2) reaction to staphylococcal exotoxins or
3) allergic response to staphylococcal antigens causing hard crusting on the eyelashes.
It is less common than seborrhoeic.
Seborrhoeic – this is a disorder of the ciliary sebaceous glands of Zeis which is associated with dandruff leading to waxy scales on the eyelashes.
Demodex infestation has also been found to be associated with blepharitis6. (Demodex Blepharitis)
Demodex are microscopic (ectoparasite) mites that live on the surface of the human body. Two types are thought to be specific to humans, Demodex folliculorum (DF) which is longer and more commonly localised to the face and Demodex brevis (DB) which are shorter and more commonly found on the neck and chest. DF are found in eyelash follicles and DB burrow deep into sebaceous and meibomian glands.
Demodex mites are also present in healthy eye lids without signs of blepharitis7.
Reports suggest that demodex act as carriers of bacteria such as staphylococcus7 and that the infestation and waste of the mites causes blockage of the follicles and glands and/or an inflammatory response2. The number of demodex mites is believed to increase with age, and over 50% of patients with demodex will have signs of blepharitis7. Treatment is needed when it becomes necessary to reduce the quantity of DB and DF and this has been shown to improve patient symptoms and ocular surface health7.
Clinical Evaluation
Risk Factors for Blepharitis
- Seborrheic dermatitis
- Infections
- Rosacea
- Allergies
- Demodex
- Dry eyes
- Long-term contact lens wear
- Cosmetics
Staphylococcal (Bacterial) Blepharitis8
Cause
- Overgrowth of Staphylococcus bacteria
- Reaction to toxins or antigens produced by the bacteria
- Chronic bacterial colonisation and biofilm formation
Signs
- Hard crusting/scales at lash base (“collarettes”)
- Lash loss (madarosis) or misdirected lashes
- Marked lid margin redness
- Telangiectasia
- Conjunctival redness
Symptoms
- Burning
- Irritation
- Foreign body sensation
- Red rim around the eyes
- Ocular discomfort
Seborrhoeic Blepharitis9
Cause
- Linked to seborrhoeic dermatitis
- Dysfunction of sebaceous glands of Zeis
- Excess oily secretions and skin flaking
Signs
- Oily/greasy deposits on lash base
- Shiny or oily eyelid margins
- Flaky skin on eyebrows/scalp/face
- Mild erythema and inflammation
Symptoms
- Tearing
- Ocular irritation
- Eyelids sticking
- Uncomfortable greasy feeling
Demodex Blepharitis10
Cause
- Infestation by Demodex mites
- D. folliculorum – lash follicles
- D. brevis – meibomian glands
- Mites carry bacteria and trigger inflammation
- Creates cylindrical collarettes (pathognomonic)
Signs
- Crusting with sleeveless clear debris encasing lashes
- Red, irritated lid margins
- Collarettes visible with magnification
- Associated with rosacea
Symptoms
- Itching (very prominent)
- Irritation
- Discomfort around eyelashes
- Persistent/stubborn inflammation
Varying degrees of ocular discomfort and or symptoms are reported but patients may also be asymptomatic.
Differences between common types of anterior blepharitis
Staphylococcal Blepharitis | Seborrhoeic blepharitis | Demodex blepharitis | |
Lashes | Lash crusting (scales at base of lashes) | Oily/greasy deposits on lid margins and around lash bases | Crusting of lashes with a cylindrical sleeve around the base of the lash extending along the lash shaft |
Loss of lashes (madarosis) | Lash loss rare | Lash loss can occur | |
Misdirection of lashes | – | – | |
Lid margin | Lid margin redness | Lid margin redness | Lid margin redness |
Eventual scarring and thickening of lid margin | Flaky skin in eyebrows | Mites under high magnification may be visible | |
Telangiectasia | – | – | |
Inflammation | Significant inflammation on lid margins | Less inflammation on lid margins | Minimal inflammation on lid margins |
Conjunctiva | Conjunctival redness | Conjunctival redness | – |
Age of patient | Typically seen in younger patients | Tends to be in older patients | Prevalence increases with age |
Skin signs | Skin is usually clear | Associated seborrhoeic dermatitis – flaky red skin | Rosacea association – red skin, telangiectasia papules and pustules |
Investigations
- Full anterior segment examination to exclude any other potential lid pathology
- Consider appearance of lid crusting to aid differential diagnosis
- Meibomian gland assessment (some practitioners find it useful to express the glands to gauge the quality and quantity of the secretions)
Management & Advice
The management of blepharitis depends on the type and severity of blepharitis11. The key to treating most types of blepharitis is keeping the lids clean and free of crusts.
The TFOS DEWS III Management and Therapy Report (2025)16 stresses that blepharitis and eyelid related dry eye must be managed using individualised, evidence based, stepwise care. Blepharitis is chronic, and long-term control depends on addressing the true source of inflammation.
Understanding the driver allows clinicians to choose treatments patients can tolerate and maintain consistently.
Non-Pharmacological
- Lid & lash cleansing: On going lid hygiene is essential for chronic eyelid conditions and tailoring frequency and specific cleansers helps maintain adherence and symptom relief
- There are a variety of lid cleansing products available to clean the crusting and debris from the lid margins and lash follicles. These products have been designed specifically for the delicate eye area. Traditionally diluted baby shampoo has been recommended for lid hygiene, but it is now known that baby shampoo can cause irritation and inflammation of the ocular surface along with adding to tear film instability12.
DEWS III highlights the need for individualised treatment algorithms — meaning the correct therapy depends on why the blepharitis is happening.
- Bacterial / Staphylococcal: benefits from antibacterial cleansing and debris removal
- Seborrhoeic: benefits from effective oil lifting cleansers
- Demodex: benefits from targeted anti-mite treatment
- Hypochlorous acid (HOCL)
- Newer management strategies for anterior blepharitis include the use of hypochlorous acid (HOCl) as an adjunct to traditional eyelid hygiene. HOCl, typically formulated at 0.01%, is applied via eyelid wipes or atomization and has demonstrated efficacy in reducing lid margin redness, abnormalities, and improving meibum expressibility and quality, with a favourable safety profile and high patient tolerability13. HOCl acts as a broad-spectrum antimicrobial, significantly reducing staphylococcal load on periocular skin without altering microbial diversity.
- Lid warming can be used prior to cleansing to soften and loosen any crusting on the lashes and may be particularly beneficial if the crusting is marked. It will also be beneficial for patients with MGD to soften thickened meibum. Commercially available warm compresses are often used for this purpose.
- Hydration/Lubrication: As dry eye is commonly present as a consequence of blepharitis patients are often recommended to include an eye lubricant as part of the management of their blepharitis. Lubricants should be instilled after the lid warming and cleansing.
Newer in practice treatment options for anterior blepharitis include microblepharoexfoliation and low-level light therapies.
Microblepharoexfoliation14 is a professional in-office procedure that mechanically removes debris, biofilm, and scurf from the eyelid margin using a rotating brush or similar device. This approach is particularly useful for patients with recalcitrant anterior blepharitis and has shown benefit in reducing symptoms and improving eyelid margin health, especially in cases associated with Demodex infestation.
Low level light therapy (LLLT)15 using blue and red wavelengths have been suggested as adjunct treatments for managing recalcitrant blepharitis, particularly in cases associated with Demodex infestations. The mechanism is thought to involve the antimicrobial and anti-inflammatory effects of blue light, which targets Demodex and associated bacteria, while red light promotes tissue repair and reduces inflammation.
These modalities are typically reserved for patients with persistent or refractory blepharitis who do not respond to conventional lid hygiene and topical therapies.
Pharmacological11
For more persistent or difficult to treat cases pharmacological options that may be considered include:
- Topical antibiotics or topical antibiotic steroid combinations that can be applied to the lid margins (e.g. Chloramphenicol, Azithromycin, Bacitracin and Erythromycin)
- Oral drugs of the tetracycline family or other systemic antibiotics (e.g. Oxytetracycline, Doxycycline, Minocycline, Lymecycline, and Azithromycin)
For Demodicosis treatments include
- Ivermectin is an antiparasitic drug and can be used orally or topically
- Metronidazole is an antibiotic and antiparasitic drug
DEWS III stresses the importance of education and adherence as core components of effective blepharitis management.
- When patients understand the cause (bacteria vs oil vs mites), adherence improves.
- Tailored plans reduce frustration and increase success with long‑term lid hygiene.
DEWS III guidance emphasises selecting interventions based on the specific pathological process, not one-size-fits-all care.
In Summary
Anterior blepharitis is a chronic inflammatory eyelid condition with multiple distinct causes: bacterial, seborrhoeic, or Demodex related.
TFOS DEWS III, encourages eyecare practitioners to identify the aetiological driver because:
- Each subtype requires different, targeted treatments
- Appropriate management improves symptom control, tear film stability, and dry eye outcomes
- Tailored care enhances patient adherence and long‑term success
Misdiagnosis can lead to suboptimal treatment and ongoing disease progression
Supporting Materials
A number of resource materials are listed below that may support you in the management of patients with blepharitis. These may help provide information to your patient in a way that promotes compliance and understanding, whilst acknowledging that time is a common restriction for clinicians in most clinical settings.
This article serves as an overview of the condition and treatment options. It does not serve as a clinical guidance. Eyecare provider guidelines should be used when managing patients.